Cutaneous T-Cell Lymphoma (CTCL) is a rare type of T-Cell Lymphoma that originates in T lymphocytes and primarily affects the skin. In this blog, we will explore its symptoms, diagnosis, treatment, prognosis, and how it fits into the broader world of lymphoma and oncology research.
What Is Cutaneous T-Cell Lymphoma (CTCL)?
Cutaneous T-Cell Lymphoma refers to a group of non-Hodgkin lymphomas in which malignant T-cells accumulate in the skin. Instead of initially affecting lymph nodes or other organs, CTCL manifests in the skin, leading to visible lesions, patches, plaques, or tumors. Because of this cutaneous (skin) involvement, it’s often referred to as “skin lymphoma.”
Two of the most common subtypes of CTCL are Mycosis Fungoides and Sézary Syndrome.
- Mycosis Fungoides is the most frequent form; it’s typically indolent (slow growing) and confined to the skin for many years.
- Sézary Syndrome is more aggressive: malignant T-cells (Sézary cells) circulate in the blood, in addition to causing widespread skin involvement.
Is Lymphoma Genetic or Hereditary?
Lymphoma is generally not considered hereditary, and most cases occur without a strong genetic link. However, a family history of lymphoma or certain inherited immune disorders may slightly increase an individual’s risk.
While Cutaneous T-Cell Lymphoma is a type of non-Hodgkin lymphoma, it’s important to recognize other blood-related conditions that may share overlapping symptoms or risk factors, such as Chronic Myeloproliferative Disease, Mantle cell Lymphoma, Follicular Lymphona. These disorders involve abnormal blood cell production and can sometimes mimic or coexist with lymphomas, highlighting the importance of accurate diagnosis and specialized hematology evaluation. Research into Follicular Lymphoma clinical trials and Mantle Cell Lymphoma Clinical Trials is ongoing and critical.
Symptoms of Cutaneous T-Cell Lymphoma (CTCL)
Understanding cutaneous t-cell lymphoma (CTCL) symptoms is vital because early stages can mimic benign skin conditions such as eczema or psoriasis. Here are key clinical features:
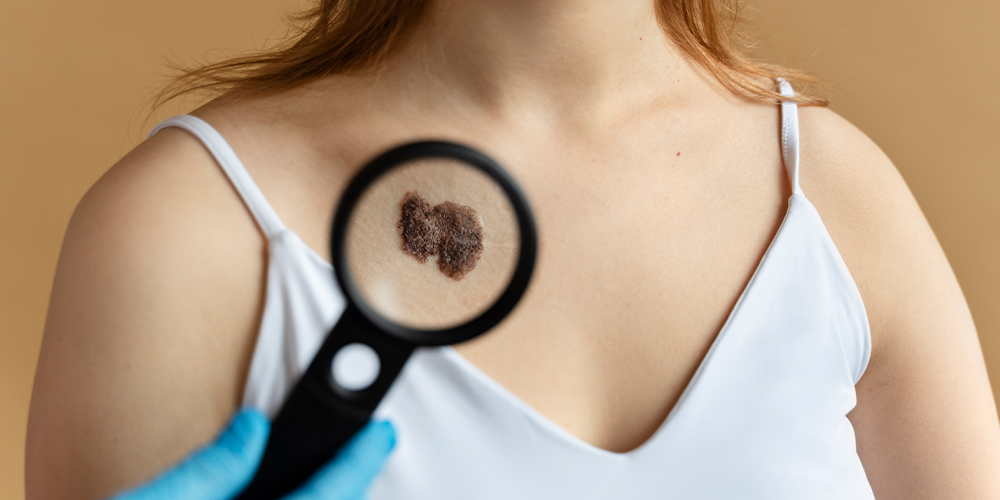
1- Red itchy skin patches: One of the hallmark signs is persistent, red, itchy patches or plaques on the skin. These can resemble dermatitis or eczema.
2- Plaques and tumors: As the disease progresses, raised plaques or even tumors may form.
3- Erythroderma: In Sézary Syndrome, patients may develop widespread redness (erythroderma) covering much of the body.
4- Blood involvement: In cases like Sézary Syndrome, malignant T-cells are found in the bloodstream, which can be detected via blood tests.
5- Lymph node or visceral involvement: In more advanced disease, lymph nodes or internal organs may be affected. Because these symptoms can be subtle and nonspecific, diagnosis is often delayed. CTCL lesions may wax and wane over years before a definitive diagnosis is made via skin biopsy.
Diagnosis and Staging
Diagnosing CTCL requires careful, multi-compartment evaluation. Clinicians look at:
- Skin (T) – size, number, type of skin lesions
- Lymph nodes (N) – if there is lymphatic spread
- Viscera (M) – internal organ involvement
- Blood (B) – presence of malignant T-cells (e.g., Sézary cells)
This is often referred to as the TNMB staging system, which helps guide treatment and predict prognosis.
Blood involvement is particularly prognostic: for example, research from PROCLIPI (Prospective Cutaneous Lymphoma International Prognostic Index) shows that even early-stage mycosis fungoides can have blood involvement (B1 status), which worsens outcomes.
Treatment Options for Cutaneous T-Cell Lymphoma
There is no universal cure for CTCL, but a variety of treatments exist to manage symptoms, control disease, and improve quality of life.
Here are common treatments:
1- Topical therapies
- Steroid creams or ointments for skin lesions.
- Other topical agents like mechlorethamine or retinoids.
2- Phototherapy / Light therapy
- Narrowband UVB or PUVA (psoralen + UVA) are frequently used, especially in early diseases.
3- Extracorporeal Photopheresis (ECP)
- A treatment particularly useful in Sézary Syndrome: blood is treated outside the body and then returned.
4- Radiation therapy
- Localized radiation for skin tumors, or total skin electron beam therapy (TSEB) in more extensive diseases.
5- Systemic therapy / Immunotherapy
- Interferon-alpha, monoclonal antibodies (e.g., mogamulizumab), and retinoids.
- Targeted therapy: for example, brentuximab vedotin in CD30+ disease.
6- Chemotherapy
- In more advanced CTCL, single-agent chemo (alkylating agents, methotrexate) or combination regimens may be used—though they are often palliative.
7- Stem cell transplant
- Allogeneic hematopoietic stem cell transplant (HSCT) can be considered in some cases, though it’s reserved for selected patients.
Hodgkin vs Non-Hodgkin Lymphoma
Lymphomas fall into two main groups: Hodgkin lymphoma and Non-Hodgkin lymphoma (NHL). Hodgkin lymphoma is identified by the presence of Reed–Sternberg cells and usually spreads in an orderly way, making it highly treatable.
Non-Hodgkin lymphoma, on the other hand, includes many subtypes—such as Cutaneous T-Cell Lymphoma (CTCL), Sézary Syndrome, and Anaplastic Large Cell Lymphoma. NHL involves either B-cells or T-cells and varies widely in behavior and prognosis.
Since CTCL is a type of non-Hodgkin lymphoma, it belongs to this larger, more diverse group.
Prognosis and Survival: Is Cutaneous T-Cell Lymphoma Deadly?
One of the most important questions patients ask is: “Is cutaneous T-cell lymphoma deadly?” The answer is nuanced.
- Many forms of CTCL, particularly early-stage Mycosis Fungoides, are indolent and not immediately life-threatening.
- According to the Cleveland Clinic, people with early-stage CTCL (Stage I or II) have a 90% 10-year survival rate.
- But in advanced diseases, prognosis worsens. For example, in late-stage (Stage III–IV), 10-year survival drops to around 53%.
- Sézary Syndrome, the leukemic variant of CTCL, has a more aggressive clinical course. The median life expectancy is significantly shorter; some sources report a median survival of 32 months.
- According to a large cohort study of aggressive CTCL, advanced Mycosis Fungoides had a 5-year survival rate of ~55%, Sézary Syndrome ~28%, and other aggressive subtypes ~33%.
Other factors also influence prognosis:
- A CTCL Severity Index (CTCL-SI) that incorporates TNM stage, lymph node, and blood involvement can predict 5-year survival more accurately.
- Age, blood involvement, large-cell transformation, elevated LDH, and more advanced stages are all linked with worse outcomes.
- According to Frontiers in Oncology, even after 32 years of follow-up, only ~2% of patients with very localized skin involvement (less than 10% of body surface) died from their disease.
Thus, while CTCL can be deadly, especially in its aggressive forms, many patients live for years or decades, especially with early diagnosis and proper management.
Living with CTCL: Quality of Life and Long-Term Management
Having cutaneous T-cell lymphoma often means dealing with chronic cancer rather than a one-time curable disease (especially in early stages). Key points for patients and caregivers:
- Regular monitoring is critical: because CTCL can progress slowly, periodic biopsies, blood tests, and skin assessments help track disease.
- Symptom management: Itching, skin discomfort, and psychosocial stress are common. Topical therapies, phototherapy, and systemic treatments help but may need to be repeated.
- Infection risk: In advanced CTCL, skin integrity may be compromised, increasing the risk of infections (e.g., Staphylococcus aureus), which is a common cause of morbidity.
- Research participation: Patients may be eligible for clinical trials, contributing to oncology research and potentially accessing cutting-edge treatments.
Why Early Detection Matters
- Because early-stage CTCL (e.g., patch or plaque stage Mycosis Fungoides) often behaves indolently, early diagnosis can allow management that maintains quality of life with minimal aggressive therapy.
- Early intervention may delay progression to more aggressive, life-threatening forms like Sézary Syndrome.
- Prognostic models (such as CTCL-SI) and staging help stratify risk and personalize care.
- Timely referral to a specialized lymphoma center or clinical research organization may open doors to clinical trials and expert multidisciplinary care.
Conclusion
Cutaneous T-Cell Lymphoma is a complex, rare form of skin lymphoma that lies at the intersection of dermatology, hematology, and oncology. While many cases, especially early Mycosis Fungoides, have favorable prognoses and can be managed over years, other variants like Sézary Syndrome or transformed disease are more aggressive and life-threatening.
Survival can range from normal life expectancy to serious outcomes, depending on subtype and stage. Clinical trials and oncology research organizations are critical for advancing therapies. CTCL often behaves as a chronic condition; ongoing care is essential for managing symptoms and preventing complications.
FAQs
Here are some of the most common questions about cutaneous T-cell lymphoma:
What are the first symptoms of Cutaneous T-cell lymphoma?
The earliest signs are often red, itchy patches or plaques on the skin that may wax and wane. Because they can mimic eczema or psoriasis, diagnosis may be delayed.
How serious is cutaneous lymphoma?
It depends. In early-stage Mycosis Fungoides, it’s often indolent and manageable, sometimes with normal life expectancy. In contrast, advanced-stage disease or Sézary Syndrome can be serious and life-shortening. Prognosis is influenced by stage, blood involvement, transformation, and patient factors.
How fast does cutaneous T-cell lymphoma spread?
CTCL typically progresses slowly over the years. Skin lesions may remain stable for long periods, especially in the early stages. However, in more aggressive forms or with blood or lymph node involvement, spread can be faster.
Is cutaneous t-cell lymphoma deadly?
Yes, it can be, particularly in its advanced or leukemic forms. But many people, especially those diagnosed early, can live for many years, and sometimes even decades, with treatment and monitoring. Survival rates vary by stage.